Otorhinolaryngology
In-game article clicks load inline without leaving the challenge.
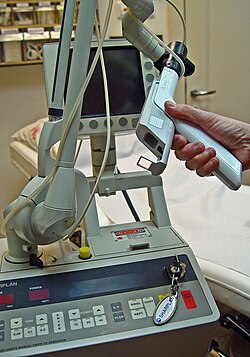

Otorhinolaryngology (/oʊtoʊˌraɪnoʊˌlærɪnˈɡɒlədʒi/ oh-toh-RY-noh-LARR-in-GOL-ə-jee, abbreviated ORL and also known as otolaryngology, otolaryngology–head and neck surgery (ORL–H&N or OHNS), or ear, nose, and throat (ENT) ) is a surgical subspecialty within medicine that deals with the surgical and medical management of conditions of the head and neck. Doctors who specialize in this area are called otorhinolaryngologists, otolaryngologists, head and neck surgeons, or ENT surgeons or physicians.
Patients seek treatment from an otorhinolaryngologist for diseases of the ear, nose, throat, base of the skull, head, and neck. These commonly include functional diseases that affect the senses and activities of eating, drinking, speaking, breathing, swallowing, and hearing. In addition, ENT surgery encompasses the surgical management of cancers and benign tumors, reconstruction of the head and neck, and plastic surgery of the face, scalp, and neck.
Etymology
The term is a combination of Neo-Latin combining forms (oto- + rhino- + laryngo- + -logy) derived from four Ancient Greek words: (cf. Greek ωτορινολαρυγγολόγος 'otorhinolaryngologist').
- οὖς (ous), 'ear', whose genitive is ὠτός (otos)
- ῥίς (rhis) 'nose'
- λάρυγξ (larynx) 'larynx'
- -λογία (logia) 'study'
Training
Otorhinolaryngologists are physicians (MD, DO, MBBS, MBChB, etc.) who complete both medical school and an average of 5-7 years of post-graduate surgical training in ORL-H&N. In the United States, trainees complete at least five years of surgical residency training. This comprises three to six months of general surgical training and four and a half years in ORL-H&N specialist surgery. In Canada and the United States, practitioners complete a five-year residency training after medical school.
Following residency training, some otolaryngologist-head & neck surgeons complete an advanced sub-specialty fellowship, where training can last for one to two years. Fellowships include head and neck surgical oncology, facial plastic surgery, rhinology and sinus surgery, neuro-otology, pediatric otolaryngology, and laryngology. In the United States and Canada, otorhinolaryngology is among the most competitive medical specialties for residency positions following medical school.
In the United Kingdom, entrance to higher surgical training is competitive. It involves a rigorous national selection process. The training programme consists of 6 years of higher surgical training after which trainees frequently undertake fellowships in a sub-speciality before becoming a consultant.
The typical total length of education, training, and post-secondary school is 12–14 years. Otolaryngology is among the more highly compensated surgical specialties in the United States. In 2022, the average annual income was $469,000.
Sub-specialties
| Head and neck oncologic surgery | Facial plastic and reconstructive surgery* | Otology | Neurotology* | Rhinology / sinus / anterior skull base surgery | Laryngology and voice disorders | Pediatric otorhinolaryngology* | Sleep medicine* |
| Surgical oncology | Facial cosmetic surgery | Ear | Middle and inner ear | Sinusitis | Voice disorders | Velopalatine insufficiency | Sleep disorders |
| Microvascular reconstruction | Maxillofacial surgery | Hearing | Temporal bone | Allergy | Phono-surgery | Cleft lip and palate | Sleep apnea surgery |
| Endocrine surgery | Traumatic reconstruction | Balance | Skull base surgery | Anterior skull base | Swallowing disorders | Airway | Sleep investigations |
| Endoscopic surgery | Craniofacial surgery | Dizziness | Apnea and snoring | Vascular malformations | |||
| Cochlear implant / BAHA | Cochlear implant/BAHA |
(*Currently recognized by American Board of Medical Subspecialties)
Topics by subspecialty
Head and neck surgery
- Head and neck surgical oncology (field of surgery treating cancer/malignancy of the head and neck) Head and neck mucosal malignancy (cancer of the pink lining of the upper aerodigestive tract) Oral cancer (cancer of lips, gums, tongue, hard palate, cheek, floor of mouth) Oropharyngeal cancer (cancer of the oropharynx, soft palate, tonsil, base of tongue) Larynx cancer (voice box cancer) Hypopharynx cancer (lower throat cancer) Sinonasal cancer Nasopharyngeal cancer Skin cancer of the head & neck Thyroid cancer Salivary gland cancer Head and neck sarcoma
- Endocrine surgery of the head and neck Thyroid surgery Parathyroid surgery
- Microvascular free flap reconstructive surgery
- Skull base surgery
Otology and neurotology
Study of diseases of the outer ear, middle ear and mastoid, and inner ear, and surrounding structures (such as the facial nerve and lateral skull base)
- Outer ear diseases Otitis externa – outer ear or ear canal inflammation Exostoses or Surfer's ear are bony growths in the outer ear canal
- Middle ear and mastoid diseases Otitis media – middle ear inflammation Perforated eardrum (hole in the eardrum due to infection, trauma, explosion, or loud noise) Mastoiditis
- Inner ear diseases BPPV – benign paroxysmal positional vertigo Labyrinthitis/Vestibular neuronitis Ménière's disease/Endolymphatic hydrops Perilymphatic fistula Acoustic neuroma, vestibular schwannoma
- Facial nerve disease Idiopathic facial palsy (Bell's Palsy) Facial nerve tumors Ramsay Hunt Syndrome
- Symptoms Hearing loss Tinnitus (subjective noise in the ear) Aural fullness (sense of fullness in the ear) Otalgia (pain referring to the ear) Otorrhea (fluid draining from the ear) Vertigo Imbalance
Rhinology
Rhinology includes nasal dysfunction and sinus diseases.
- Nasal obstruction Inferior turbinate hypertrophy Nasal septum deviation Chronic sinusitis with nasal polyps
- Sinusitis – acute, chronic
- Environmental allergies
- Rhinitis
- Pituitary tumor
- Empty nose syndrome
- Severe or recurrent epistaxis
Pediatric otorhinolaryngology
- Adenoidectomy
- Caustic ingestion
- Cricotracheal resection
- Decannulation
- Laryngomalacia
- Laryngotracheal reconstruction
- Myringotomy and tubes
- Obstructive sleep apnea – pediatric
- Tonsillectomy
Laryngology
- Dysphonia/hoarseness Laryngitis Reinke's edema Vocal cord nodules and polyps
- Spasmodic dysphonia
- Tracheostomy
- Cancer of the larynx
- Vocology – science and practice of voice habilitation
- Muteness and selective muteness
Facial plastic and reconstructive surgery
Facial plastic and reconstructive surgery is a one-year fellowship open to otorhinolaryngologists who wish to begin learning the aesthetic and reconstructive surgical principles of the head, face, and neck pioneered by the specialty of Plastic and Reconstructive Surgery.
- Rhinoplasty and septoplasty
- Facelift (rhytidectomy)
- Browlift
- Blepharoplasty
- Otoplasty
- Genioplasty
- Injectable cosmetic treatments
- Trauma to the face Nasal bone fracture Mandible fracture Orbital fracture Frontal sinus fracture Complex lacerations and soft tissue damage
- Skin cancer (e.g. Basal Cell Carcinoma)
Sleep surgery
Sleep surgery encompasses any surgery that alleviates obstructive sleep apnea and can anatomically include any part of the upper airway.
- Nasal cavity / nasopharynx Septoplasty Adenoidectomy (especially in pediatrics)
- Oral cavity / oropharynx Tonsillectomy (especially in pediatrics) Uvulopalatopharyngoplasty Transoral midline glossectomy Genioglossus advancement
- Other Hyoid suspension Maxillomandibular advancement Hypoglossal nerve stimulation
Microvascular reconstruction repair
Microvascular reconstruction repairs are commonly performed on patients consulting an otorhinolaryngologist. It is a surgical procedure that involves moving a composite piece of tissue from the patient's body to the head and/or neck. Microvascular head-and-neck reconstruction is used to treat head-and-neck cancers, including those of the larynx and pharynx, oral cavity, salivary glands, jaws, calvarium, sinuses, tongue, and skin. The tissue most commonly moved during this procedure is from the arms, legs, and back, and can come from the skin, bone, fat, and/or muscle.
When performing this procedure, the reconstructive needs determine which is moved. Transfer of the tissue to the head and neck allows surgeons to rebuild the patient's jaw, optimize tongue function, and reconstruct the throat. When pieces of tissue are moved, they require their own blood supply to survive in their new location. After the surgery is completed, the blood vessels that feed the tissue transplant are reconnected to new blood vessels in the neck. These blood vessels are typically no more than 1 to 3 millimeters in diameter, which means that these connections need to be made with a microscope, which is why the procedure is called "microvascular surgery".[citation needed]